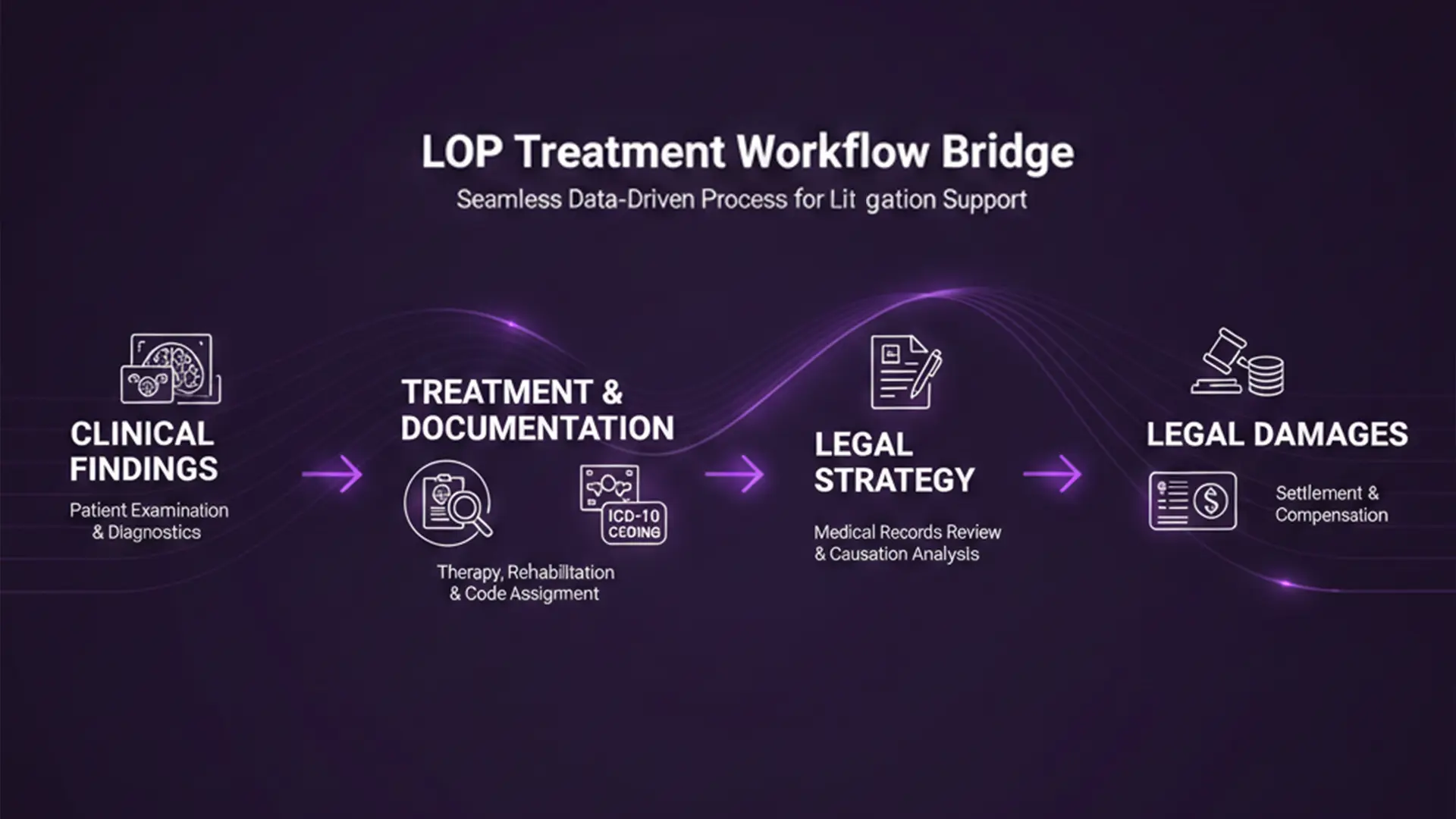
An LOP treatment workflow is a medical-legal collaboration system allowing injured complainants to access specialized care without upfront costs, postponing payment until the claim’s resolution. Strategically, this workflow serves as the primary evidentiary engine of a personal injury case, converting clinical interventions into a narrative designed to withstand the evaluation of insurance adjusters and algorithmic models. It is the bridge between clinical findings and an attorney’s ability to prove damages in a quantifiable manner.
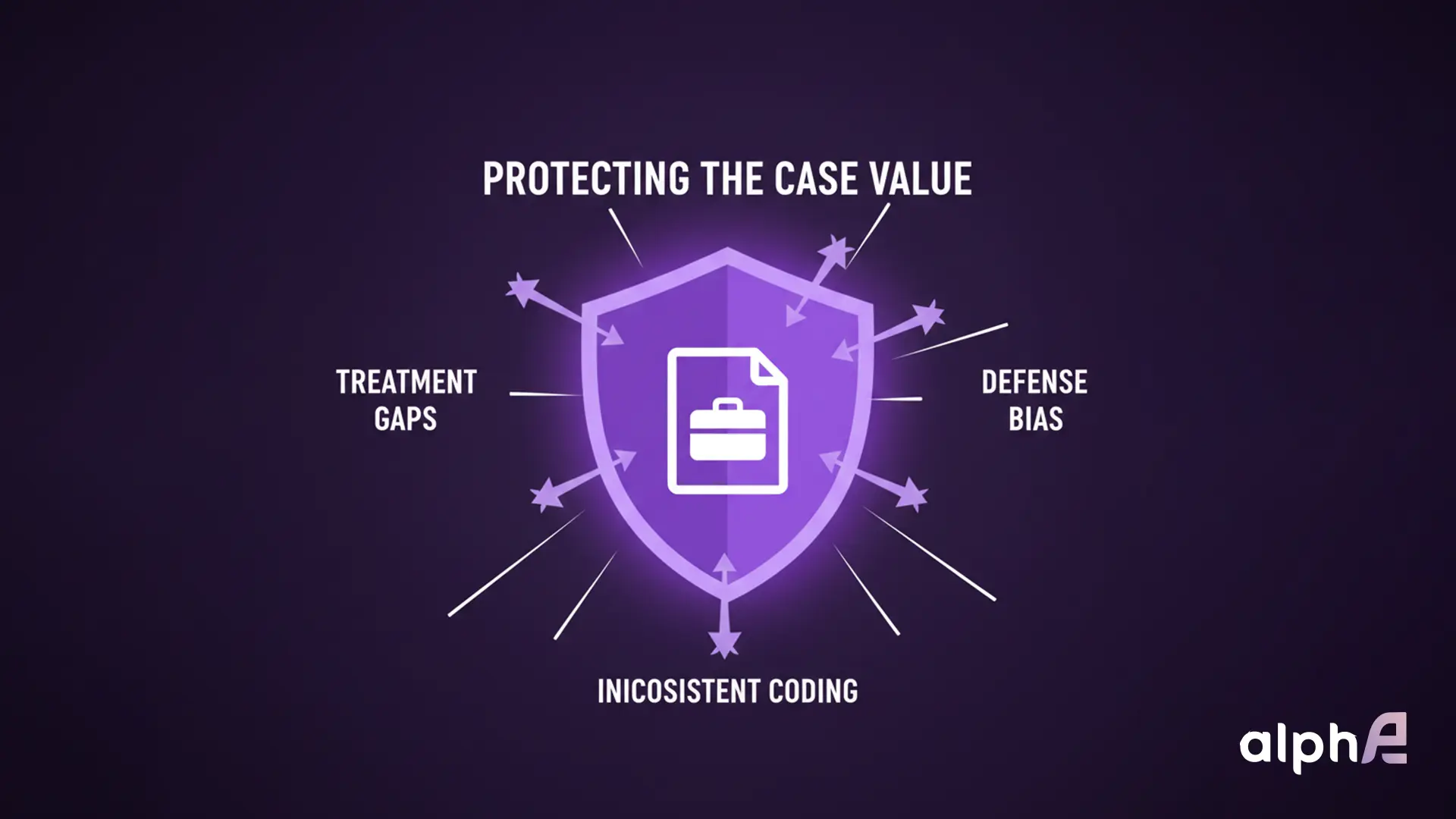
For the personal injury attorney, the letter of protection treatment process is a mechanism for managing claim “credibility.” By centralizing oversight, firms ensure diagnostic timing and documentation quality align with the “reasonable and necessary” standards needed for recovery under Texas law, mollifying “friction points” like treatment gaps or inconsistent coding.
While frequently viewed as an accounting tool, high-growth practices recognize this medical workflow as a data-generation tool that feeds the internal logic of adjustment software. If data points, from therapy frequency to ICD-10 codes, are unsynchronized, the claim is flagged as “low-value” before a human adjuster reviews the file.
Intake Strategy and Early-Stage Risk Analysis
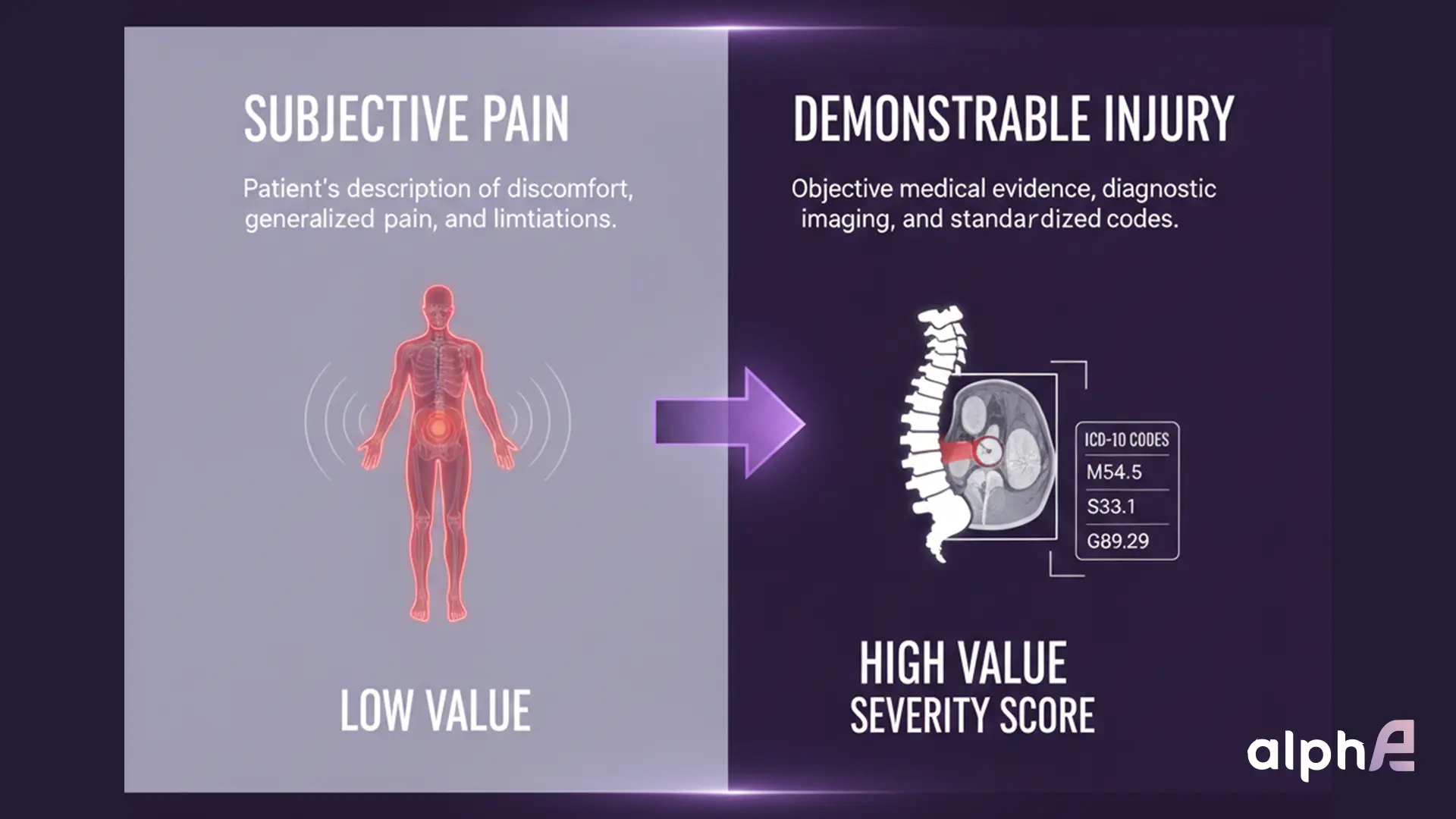
The true value of managing LOP medical cases is determined long before a demand letter is drafted; it is established during the initial intake and triage phase. At this stage, a strategic risk analysis must assess the injury’s “demonstrable” versus “nondemonstrable” nature. Insurance adjustment software, such as Colossus, utilizes approximately 600 injury codes, prioritizing “demonstrable” injuries that can be objectively verified through imaging, specifically X-rays, MRIs, or CT scans, over subjective reports of pain.
Distinguishing Demonstrable vs. Non Demonstrable Injuries
A flawed LOP treatment workflow fails by allowing treatment gaps or failing to link the injury mechanism to the diagnostic pathway. In algorithmic evaluation, a gap is a “value reset,” suggesting the injury has resolved. Strategic intake ensures the clinical pathway mirrors the legal necessity of objective proof across three pillars:
- Diagnostic Linkage: Ensuring that initial complaints of “non-demonstrable” pain, such as soft tissue trauma or traumatic brain injury (TBI), are immediately followed by specialized neurological or orthopedic evaluations to establish objective clinical findings. This linkage converts a “subjective” complaint into a “severity point” within the insurer’s valuation model.
- Provider Matching and Algorithm Weighting: Selecting specialists (e.g., neurosurgeons vs. chiropractors) based on how their documentation is weighted by valuation algorithms.
- Liability-Causation Integrity: Analyzing whether the medical narrative can distinguish new trauma from pre-existing degenerative conditions. This is a frequent tactical target used by the defense to devalue claims in litigation.
The Strategic Cost of “Friction Points”
The goal of managing LOP medical cases is to eliminate ambiguity. If a workflow delays an EMG for radiating pain, the claim remains categorized as “soft tissue.” Front-loading diagnostic rigor secures the evidentiary foundation necessary for high-leverage negotiations.
Strategic Positioning: Documentation as Valuation Leverage
In the personal injury landscape, the primary value of how LOP medical treatment works lies in the production of “attorney-ready” documentation that simplifies the adjuster’s data-entry process. Insurance adjusters, often lacking specialized medical training, rely on automated systems to second-guess a treating physician’s prognosis. When an LOP-based care coordination produces fragmented or delayed records, it provides adjusters with the technical justification to arbitrarily reduce settlement offers based on “insufficient documentation.”
Transitioning from Billing-Focused to Litigation-Focused Workflows
Strategic positioning requires a move away from “billing-focused” LOPs toward “litigation-focused” workflows. Documentation must accurately reflect the clinical severity and objective findings that valuation systems recognize when assessing claim value. For example, the duration and frequency of physical therapy are often categorized by insurers into specific time ranges (e.g., 30 days vs. 31 days). Certain treatment duration thresholds may influence how valuation systems interpret the overall severity and persistence of injury, particularly when supported by consistent clinical documentation.
Insurer Interpretation of LOP-Based Medical Narratives
The defense often views the LOP provider not as a disinterested clinician but as an “investor” in the litigation. This “investor bias” is a primary tactical target; defense counsel will attempt to frame the provider’s financial stake in the settlement as a conflict of interest that compromises clinical objectivity.
The Texas Transparency Shift
In Texas, the discoverability of these arrangements has shifted toward total transparency. Following the precedents set in, the defense is now entitled to discover a provider’s negotiated rates with private insurers to challenge the “reasonableness” of LOP billing.
Consequently, an LOP treatment workflow must account for this visibility. If a narrative relies on chargemaster rates without a defensible clinical rationale, the claim becomes vulnerable to “paid vs. incurred” disputes under Section 41.0105 of the Texas Civil Practice and Remedies Code. Strategic management of LOP medical cases requires a narrative that emphasizes medical necessity to insulate the file against these cost-containment arguments.
Navigating Rules-Based Adjustment Models
To maximize valuation, the letter of protection treatment process and a deep understanding of how LOP medical treatment works must be calibrated to the specific logic of rules-based systems like Colossus, Claims Outcome Advisor, and Claims IQ. These programs convert medical inputs into a numeric “severity score” using thousands of internal valuation rules designed to standardize claim assessments and reduce subjectivity.
Understanding how LOP medical treatment works within these models reveals that the sequence of treatment is as vital as the treatment itself. For instance, a specialist consultation scheduled midway through a physical therapy course can “reset” the value of therapy visits in the eyes of the algorithm, which might otherwise depreciate those visits as time progresses.
Key algorithmic drivers include:
- Demonstrable Impairment: Positive MRI findings for herniated discs or nerve compression carry significantly higher severity multipliers than subjective “strain/sprain” diagnoses.
- ICD Code Optimization: While providers use thousands of codes, Colossus prioritizes approximately 600. A workflow ensuring providers use “demonstrable” codes supported by objective diagnostics naturally yields higher valuations.
- Medication and Appliances: The prescription of specific medical appliances (like back braces or TENS units) or certain classes of medication can trigger additional severity points within the system.
When managing LOP medical cases, the objective is to supply the specific data points these unfeeling systems require while documenting the lifestyle impact necessary for an attorney to later overcome algorithmic limitations during human negotiations.
Mitigating Friction Points in Complex Narratives
Fragmented workflows provide insurance defense with the opportunity to challenge the necessity of medical care. In complex cases involving multi-level spinal trauma or brain injury, the narrative must be longitudinal and interdisciplinary. Any interruption in the letter of protection treatment process, whether due to scheduling conflicts or financial friction, is interpreted by adjusters as evidence that the injury has resolved. To mitigate these risks, the treatment workflow must prioritize:
- Continuity of Care: Preventing treatment gaps that “reset” the insurer’s valuation clock.
- Causation-Focused Reporting: Ensuring specialists explicitly link clinical findings to the specific accident mechanism.
- Billing Integrity: Avoiding “dual chargemasters” or upcoding that forensic experts exploit during discovery to undermine the legal strategy.
At alphaE, we specialize in refining these medical-legal narratives to ensure that complex orthopedic injuries and other high-stakes claims are positioned for maximum valuation leverage. Our strategic approach bridges the gap between clinical documentation and the algorithmic requirements of insurance adjustment software, transforming potential liabilities into evidentiary assets. By aligning your firm’s digital authority with data-driven case positioning, we help you overcome the friction points that characterize the modern insurance defense playbook.
Texas Legal Context for LOP Workflows
LOP-based medical coordination in Texas operates within a well-defined legal framework governing billing transparency, evidentiary standards, and the recoverability of medical expenses. The following authorities are particularly relevant to how courts evaluate reasonableness, necessity, and financial bias in personal injury litigation:
Texas Civil Practice & Remedies Code § 41.0105
Governs recovery of medical expenses based on the net amount actually paid or incurred (“Paid vs. Incurred”).
Texas Civil Practice & Remedies Code § 18.001
Establishes the affidavit process for proving the reasonableness and necessity of medical services.
In re K & L Auto Crushers, LLC, 627 S.W.3d 239 (Tex. 2021)
Addresses the discoverability of negotiated provider rates and billing transparency in personal injury cases.
Texas Rule of Civil Procedure 192.3
Understanding this legal landscape is essential when structuring an LOP treatment workflow that prioritizes clinical integrity, defensible billing practices, and litigation-ready documentation.