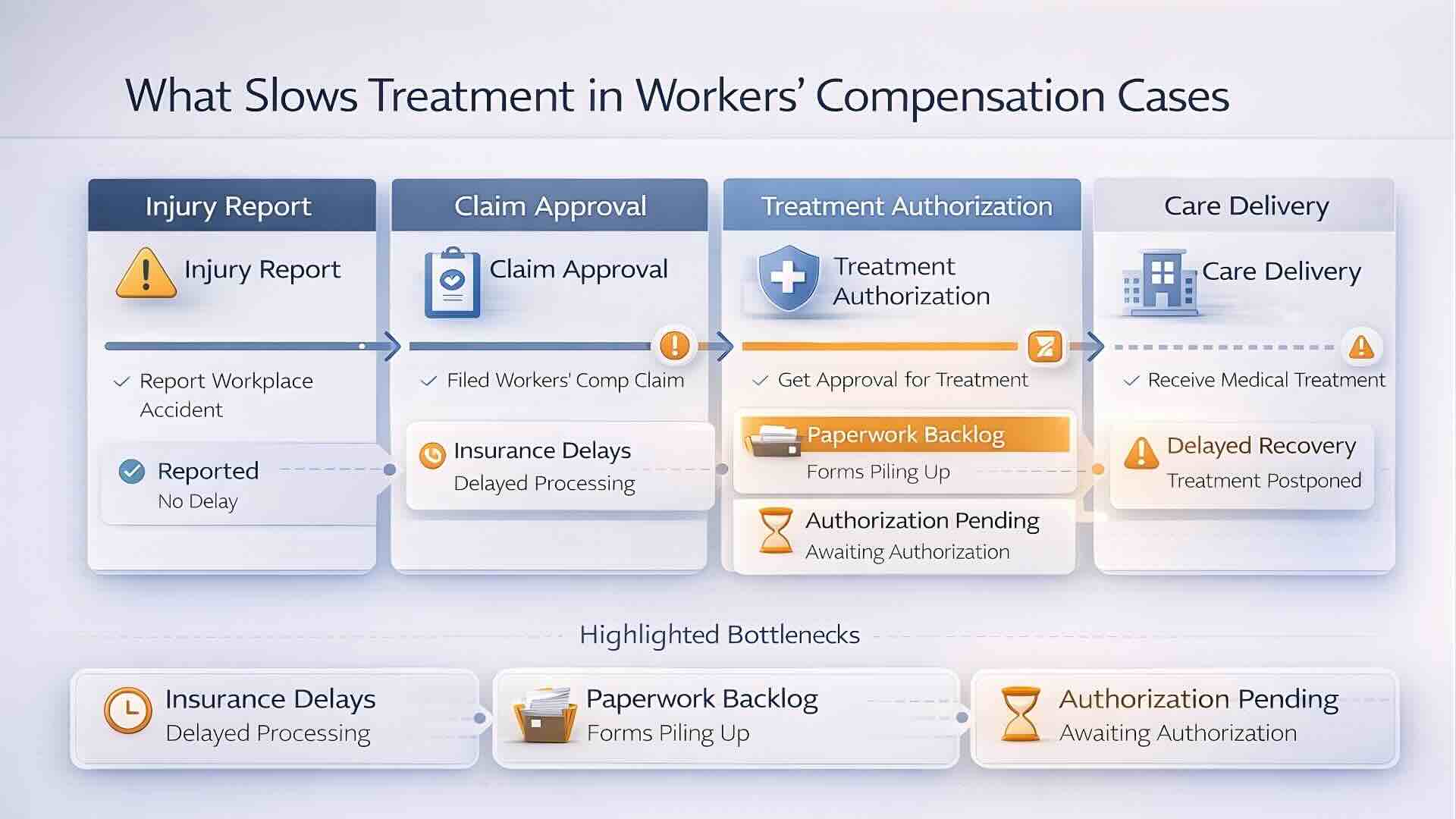
In a workers’ compensation case, treatment delays rarely begin with one obvious breakdown. More often, they start with small points of friction a missed detail, a late authorization, a provider mismatch, or records that do not clearly connect the injury to the care being requested. By the time the delay becomes visible, the worker is still in pain, the medical timeline is harder to support, and the case is already more difficult to move forward.
For firms handling these claims, the issue is not simply whether treatment was eventually provided. It is whether the care path stayed clear, medically supported, and documented well enough to keep the file progressing. In many cases, treatment slows down because timing, medical necessity support, provider coordination, and communication all have to stay aligned at the same time.
Why Treatment Delays Often Start Before a Formal Denial
Treatment often begins to slow down before anyone formally calls it a denial. In Texas workers’ compensation cases, delays can start during preauthorization, utilization review, or disputes over medical necessity. When a carrier questions whether a service is necessary, the file may move into reconsideration or Independent Review Organization review, adding more time before care can continue.
Research has shown that longer delays in access to care are associated with worse recovery patterns and longer periods of work disability in compensated musculoskeletal cases. For law firms and case-coordination teams, the takeaway is practical: once treatment starts drifting, the medical timeline becomes harder to support and the case becomes harder to move forward. Delays should be addressed early as a coordination issue, not left to grow into a larger documentation or administrative problem.
Delays should be addressed early as a coordination issue, not left to grow into a larger documentation or administrative problem especially in cases that require structured medical coordination for workers’ compensation cases.
Common Causes of Treatment Delays in Workers’ Compensation Files
Most workers’ compensation files do not stall for unusual reasons. In most cases, delays build because a few recurring bottlenecks stack on top of each other. The most common include:
Authorization and utilization review friction. Requests for imaging, specialist care, therapy, injections, or surgery may sit in review longer than expected, especially when medical necessity support is limited.
Provider mismatch. A worker may be sent to a clinic that is not the right fit for the injury, the claim environment, or the documentation demands of the file.
Incomplete or inconsistent records. When the diagnosis, mechanism of injury, restrictions, and treatment rationale are not tied together clearly, the file becomes easier to challenge.
Referral sequencing problems. Delays often grow when follow-up care, imaging, and specialty referrals are not lined up in the right order.
Claim-processing disputes. Compensability questions, body-part disputes, or disagreement about work-relatedness can stall care before the medical issues are fully addressed.
Even basic administrative errors can create access problems. Research has shown that claim denials and temporary denials are sometimes linked to incorrect carrier information, which highlights how easily treatment can be delayed when core claim details are not handled cleanly.
Why Early Documentation Quality Affects Treatment Speed
Good documentation does more than preserve the record. It can directly affect how quickly treatment decisions move forward. When an initial evaluation clearly explains how the injury happened, what objective findings support the diagnosis, what restrictions apply, and why the next step in care is medically necessary, there is less room for avoidable back-and-forth.
In many workers’ compensation files, treatment does not slow down because the medical issue is unclear. It slows down because the file does not explain the medical need clearly, early, and consistently. When documentation leaves gaps around mechanism of injury, diagnosis support, functional limitations, or treatment rationale, each next step becomes easier to question and harder to approve.
What strong early records usually need to show
A useful early record answers the key questions without forcing an adjuster, reviewer, or downstream specialist to guess. It should explain what happened, how the mechanism relates to the reported injury, what findings support the diagnosis, what treatment has already occurred, how the worker responded, and why the next requested service is medically reasonable at that stage. It should also connect restrictions, follow-up timing, and referral sequencing in a way that makes the file easy to follow.
When those points are scattered across disconnected notes, workers compensation treatment delays become more predictable because every next step has to be reconstructed instead of supported.
Why Provider Selection Has a Direct Impact on Treatment Speed
The first provider can shape almost everything that follows in a workers’ compensation case. A poor provider match can lead to delayed appointments, weak documentation, or treatment plans that do not align with the demands of the claim. In many cases, these issues are not immediately visible, but they begin to affect the file as the case progresses.
Providers who are not experienced in injury-related cases may struggle to document mechanism of injury, functional limitations, or treatment rationale in a way that supports continued care. They may also delay referrals, under-document progression, or fail to align treatment with claim requirements, which can slow down the entire process.
In practice, treatment delays often begin with a referral decision that seemed acceptable at intake but did not match the actual complexity of the injury or the documentation demands of the case. Selecting the right provider early is one of the most direct ways to reduce downstream delays.
Selecting the right provider early is one of the most direct ways to reduce downstream delays, which is why firms should understand how PI attorneys should vet medical providers early before sending a case into treatment.
What delay looks like in a real case timeline
Most treatment problems do not begin as a clear crisis. They usually appear as gradual drift in the timeline. A worker reports a lifting injury. The first visit documents pain but not enough functional detail. Therapy is started, but progress is vague. Imaging is requested late. The referral to a specialist does not happen until symptoms have persisted for weeks. By then, the carrier is asking sharper questions, the worker is frustrated, and the file is harder to move forward. That is how workers compensation treatment delays tend to accumulate in ordinary cases.
Signs the file is already starting to slow down
- Follow-up appointments are happening, but the treatment plan is not advancing.
- Notes repeat symptoms without clarifying functional change or medical rationale.
- Referrals are discussed informally but not scheduled promptly.
- Diagnostic requests arrive after conservative care has already lost momentum.
- Different providers describe the injury in ways that do not line up cleanly.
When firms ask why workers comp treatment gets delayed, this is often the answer they find: not one catastrophic failure, but a file that slowly becomes harder to support at each step.
How to reduce delay before the file becomes harder to recover
The best response is usually practical, not theoretical. Once a workers’ compensation case starts lagging, the team needs a tighter treatment path, clearer communication, and more disciplined follow-up.
- Match the provider to the injury and claim environment early. Do not treat every musculoskeletal injury as interchangeable.
- Set expectations for documentation from the first visit. Mechanism, diagnosis, function, restrictions, and next-step rationale need to connect.
- Track referral timing aggressively. Specialty care, imaging, and follow-up should not depend on passive reminders.
- Watch for treatment drift. If the plan is repeating without progress, the file likely needs a more deliberate next step.
- Keep the medical story organized across providers. Consistency matters when utilization review or dispute review enters the picture.
This is also the point where internal coordination becomes especially valuable. As outlined on the alphaE website, the focus is on helping law firms keep treatment organized, maintain accessible records, and ensure communication flows smoothly between providers and legal teams. That approach reflects a key reality in delayed treatment in workers compensation cases: the issue is often logistical, not just legal or medical.
For firms building a more disciplined referral process, understanding how to vet LOP medical providers can serve as a practical benchmark, especially when provider fit, appointment timing, and documentation reliability directly affect case progression.
Conclusion
For firms trying to reduce avoidable treatment friction, it also helps to understand how alphaE helps law firms keep treatment and documentation organized across the life of an injury case.
The main lesson is that many of the most damaging delays are foreseeable. Delayed treatment in workers compensation cases usually grows out of administrative friction, weak documentation, referral lag, or provider mismatch long before the file reaches a formal dispute stage. Once that happens, recovery slows, records get harder to defend, and the claim becomes heavier for everyone involved.
A stronger approach starts earlier, because workers compensation treatment delays are easier to prevent than unwind. When firms tighten provider selection, protect documentation quality, and keep treatment steps moving in sequence, they reduce the chance that workers compensation treatment delays will shape the outcome of the file.
For teams that handle medically complex injury matters, that kind of coordination is not a nice extra. It is part of how treatment stays credible and how the case keeps moving. In that sense, workers compensation treatment delays are often a warning sign that the file needs better structure, faster follow-through, and clearer medical support. From that perspective, the real question is how early the team recognizes the pattern and corrects it before the file loses more ground.